Welcome to our project
Our objectives are to develop a prototype for a sleep oxygen level monitor and a website to assess the risk of obstructive sleep apnea.
What is OSA ?
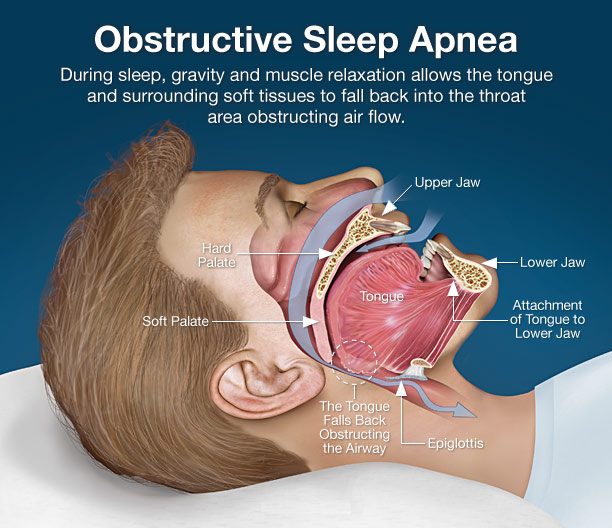
In general, men are 2 to 3 times more likely as premenopausal women to have obstructive sleep apnea. However, the risk of obstructive sleep apnea increases in women after menopause. A family history of sleep apnea. Having family members with obstructive sleep apnea might increase your risk.
OSA stand for Obstructive Sleep Apnea
- Symptoms
- Loud snoring.
- stop breathing during sleep.
- Gasping for air during sleep.
- Feeling tired or even exhausted when waking up.
- Difficulty staying asleep, known as insomnia.
- Excessive daytime sleepiness, known as hypersomnia.
This is the more common form. Obstructive sleep apnea happens when muscles in your head and neck relax while you’re asleep, causing the surrounding tissue to press on your windpipe. That obstructs air’s ability to pass through it.
- Causes
- obesity hypoventilation syndrome, a breathing disorder in people with obesity
- endocrine conditions, such as hypothyroidism, acromegaly, and polycystic ovary syndrome, which may affect your breathing when you’re asleep
- chronic lung disease, such as asthma, chronic obstructive pulmonary disease (COPD), and pulmonary fibrosis
- neuromuscular conditions, such as a stroke, which can interfere with brain signals to your chest muscles and airway
- heart or kidney failure, which may cause fluid to build up in your neck and obstruct the upper airway
ODI Calculator
ODI rate
BMI Calculator
OSA Risk Assessment

- ODI refers to the average number of desaturation episodes occurring per hour, where desaturation episodes are defined as a decrease in the mean oxygen saturation( we use 98% as the baseline SpO2 in this project ) of ≥3% that lasts for at least 10 seconds.
- ODI was graded into three groups: mild (5-15), moderate (15-30), and severe (≥30) OSA. Patients with an ODI < 5 were graded as having no oxygen desaturation.
- the relationship between OSA and hypertension
- The Wisconsin Sleep Cohort provided the earliest notable evidence of a dose–response relationship between obstructive sleep apnea (OSA) and hypertension. In this landmark study, 1,060 asymptomatic participants underwent overnight polysomnography (in-laboratory sleep studies) to assess the presence and severity of OSA. The investigators found a dose–response relationship between the severity of obstructive sleep apnea (OSA) and the likelihood of developing hypertension in this study cohort.
- OSA and arrhythmia
- Patients with obstructive sleep apnea (OSA) are more likely to experience sudden death during the night compared to those without OSA, highlighting an increased risk of arrhythmias. Additionally, the connection between OSA and atrial fibrillation may contribute to the higher risk of stroke seen in these patients.
- OSA and coronary artery disease
- Mooe et al. found that obstructive sleep apnea (OSA) is independently associated with a worse prognosis in patients with coronary artery disease (CAD). Recent large studies have also demonstrated this link between untreated OSA and an increased risk of both fatal and nonfatal cardiovascular events.